Knee Hurts When Bent: Causes, Tips, and Relief
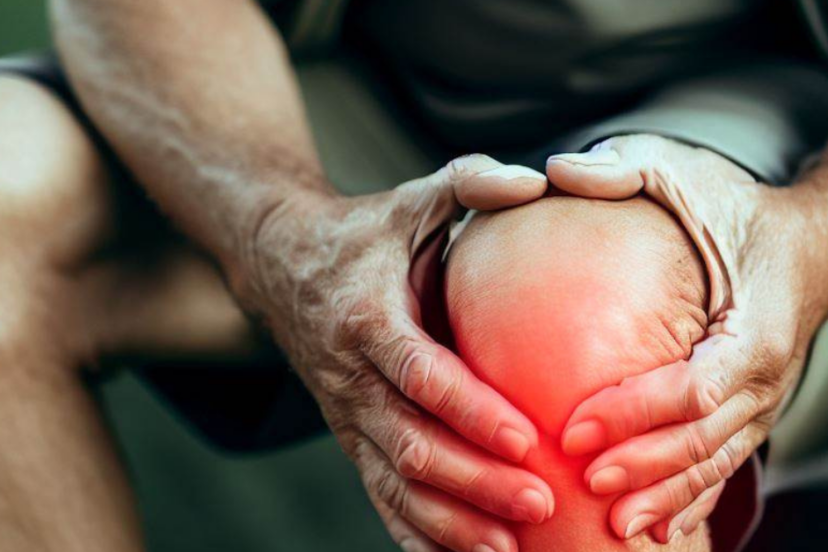
Have you ever experienced pain in your knee when bending it? Don’t worry; you’re not alone. Many people encounter knee discomfort or even sharp stabbing pain in the knee when flexing their knees. In this article, we’ll explore the reasons behind knee pain when bent and provide you with helpful suggestions to find relief.
When your knee hurts when bent, it can significantly impact your daily activities and quality of life. Understanding the underlying causes of this discomfort is crucial to effectively address the issue and prevent further complications.
Understanding Knee Anatomy : Why Knee Hurts When Bent
To comprehend why the knee may hurt when bent, let’s take a closer look at the knee’s complex anatomy. The knee joint consists of various structures, including bones, ligaments, tendons, and cartilage. Bending the knee involves intricate interactions between these components.

The knee is one of the most vital and complex joints in the human body. It facilitates various movements, from walking and running to jumping and squatting. Understanding the intricate anatomy of the knee is crucial for maintaining its health and preventing injuries. In this article, we will delve into the components that form the knee joint, their functions, and how they work together to provide stability and support.
Bones of the Knee
The knee joint is formed by three bones: the femur (thigh bone), tibia (shin bone), and patella (kneecap). The rounded end of the femur sits on the flat surface of the tibia, and the patella glides along the femur’s groove.
Ligaments
Ligaments are strong bands of connective tissue that hold the bones of the knee joint together. The four main ligaments in the knee are:
1. Anterior Cruciate Ligament (ACL): Prevents the femur from sliding backward on the tibia and provides stability during rotational movements.
2. Posterior Cruciate Ligament (PCL): Prevents the femur from sliding forward on the tibia and provides stability during rotational movements.
3. Medial Collateral Ligament (MCL): Supports the inner side of the knee and prevents the knee from bending inward.
4. Lateral Collateral Ligament (LCL): Supports the outer side of the knee and prevents the knee from bending outward.
Tendons
Tendons are tough, fibrous tissues that connect muscles to bones. The quadriceps tendon connects the quadriceps muscle to the patella, and the patellar tendon connects the patella to the tibia. These tendons play a vital role in knee extension and movement.
Cartilage
Articular cartilage is a smooth, slippery tissue that covers the ends of the femur, tibia, and back of the patella. It allows the bones to glide smoothly against each other during knee movement, reducing friction and preventing wear and tear.
Menisci
The knee contains two menisci – the medial meniscus on the inner side and the lateral meniscus on the outer side. These C-shaped pieces of cartilage act as shock absorbers, distributing forces evenly across the knee joint and enhancing joint stability.
Synovium
The synovium is a thin, delicate lining within the knee joint capsule. It produces synovial fluid, which lubricates the joint and nourishes the cartilage, promoting smooth movement.
Bursae
Bursae are fluid-filled sacs located near the knee joint. They reduce friction between tendons, ligaments, and bones, helping to prevent irritation and inflammation.
Functions of the Knee
The knee joint enables essential movements, including flexion (bending), extension (straightening), and rotation. It supports the body’s weight during standing and walking, absorbs impact during activities, and provides stability for various dynamic movements.
The knee is a remarkable and intricate joint that plays a crucial role in human mobility. Understanding its anatomy is essential for maintaining knee health and preventing injuries. The combination of bones, ligaments, tendons, cartilage, and other components allows the knee to function efficiently, supporting our daily activities and active lifestyles. Proper care, exercise, and precautionary measures can help keep the knee joint strong and resilient throughout life.
Common Causes of why Knee Hurts When Bent
There are several potential causes for knee pain when bent. Some common conditions include:
1. Patellofemoral Pain Syndrome: This condition occurs when the kneecap doesn’t properly align with the thigh bone, resulting in pain when bending the knee.
2. Meniscal Tear: A tear in the meniscus, which is the cartilage that cushions the knee joint, can cause pain and discomfort during knee flexion.
3. Osteoarthritis: Knee osteoarthritis often leads to pain, stiffness, and limited mobility, especially when bending the knee.
4. Ligament Sprains: Injuries to the knee ligaments, such as the anterior cruciate ligament (ACL) or medial collateral ligament (MCL), can cause pain and instability when bending the knee.
Identifying the specific cause of your knee pain is essential for determining the appropriate treatment and management strategies. Lets dive into each common cause in more detail:
1. Defeating Patellofemoral Pain Syndrome

Empowering You to Conquer the Challenge of Knee Discomfort and Rediscover Active Living!
Patellofemoral Pain Syndrome (PFPS), often referred to as “runner’s knee,” is a common condition that affects individuals of all ages and activity levels. It manifests as pain around the kneecap, resulting from the improper tracking of the patella (kneecap) along the femoral groove during movement. As an enthusiast and advisor in the realm of PFPS, I understand the impact it can have on one’s life. In this article, I’ll provide valuable insights, helpful suggestions, and reasons to conquer PFPS and resume an active, pain-free lifestyle.
Understanding PFPS
To effectively address PFPS, it’s crucial to comprehend the intricate anatomy and function of the patellofemoral joint. This joint allows for smooth movement during activities like walking, running, and jumping. Several factors can contribute to PFPS, including overuse, muscle imbalances, biomechanical issues, and previous injuries. Common symptoms include localized knee pain, discomfort when climbing stairs or sitting for extended periods, and a grinding sensation in the knee.
Diagnosing PFPS
If you suspect PFPS, seeking medical evaluation is essential. A healthcare professional will conduct a thorough examination and gather your medical history to make an accurate diagnosis. Imaging and diagnostic tests, such as X-rays and MRIs, may be utilized to rule out other conditions and confirm PFPS.
Managing PFPS
Fortunately, most cases of PFPS can be effectively managed with conservative treatments. Rest and activity modification are crucial during the initial phase of recovery. Physical therapy plays a vital role in strengthening the muscles around the knee and improving flexibility. Employing RICE (Rest, Ice, Compression, Elevation) can help reduce inflammation and alleviate pain. Pain management techniques, such as non-steroidal anti-inflammatory drugs (NSAIDs), may provide relief.
Preventive Measures
Prevention is better than cure. Adopting preventive measures can reduce the risk of PFPS recurrence. Proper warm-up and cool-down routines before and after physical activity can prepare the body and prevent sudden strain. Maintaining a healthy body weight can minimize stress on the knees. Choosing appropriate footwear with adequate support and cushioning is essential for reducing impact during exercise. Gradually increasing physical activity can prevent overuse injuries.
Tips for Living with PFPS
Living with PFPS doesn’t have to be restrictive. Making lifestyle modifications, such as avoiding high-impact activities and opting for low-impact alternatives like swimming or cycling, can help manage symptoms. Addressing the psychological and emotional aspects of PFPS is equally crucial. Staying positive and seeking support from healthcare professionals and loved ones can improve overall well-being.
Conquering Patellofemoral Pain Syndrome is possible with the right approach and guidance. Armed with an understanding of PFPS, implementing appropriate treatments, and adopting preventive measures, you can reclaim an active life free from knee discomfort. Remember, your journey to recovery is unique, and with determination and support, you can triumph over PFPS and embrace an empowered, pain-free existence. Further Scientific Study shows strengthening through weight-bearing and non–weight bearing exercises is a common component of the rehabilitation program.
2. Meniscal Tear

Understanding, Treating, and Recovering from this Common Knee Injury
A meniscal tear is a prevalent knee injury that affects individuals of all ages and activity levels. The menisci are C-shaped, rubbery cartilage discs that act as shock absorbers between the thighbone (femur) and shinbone (tibia). They play a crucial role in providing stability and cushioning to the knee joint during movement. However, sudden twists, repetitive movements, or degeneration over time can lead to meniscal tears. In this article, we will delve into the causes, symptoms, diagnosis, treatment options, and recovery process for meniscal tears.
Understanding Meniscal Tears
Meniscal tears can occur due to various factors, such as sudden trauma during sports activities or degeneration associated with age-related wear and tear. Athletes involved in contact sports, such as football and basketball, are particularly susceptible to meniscal injuries. Older adults may experience meniscal tears due to the natural aging process, which can weaken the cartilage.
Symptoms of Meniscal Tears
Meniscal tears can present with a range of symptoms, including pain, swelling, stiffness, and a sensation of catching or locking in the knee joint. Patients may also experience difficulty in fully extending or flexing the knee. Some individuals might notice a clicking sound or sensation during movement. If you experience any of these symptoms, seeking prompt medical attention is crucial for an accurate diagnosis and timely treatment.
Diagnosing Meniscal Tears
A thorough evaluation by a healthcare professional is essential for diagnosing a meniscal tear. The examination may include a review of your medical history, a physical examination to assess knee movement and stability, and imaging tests such as MRI or X-rays to confirm the diagnosis. These tests allow doctors to assess the extent and location of the tear accurately.
Treatment Options
The appropriate treatment for a meniscal tear depends on several factors, including the type and location of the tear, as well as the patient’s age and activity level. In some cases, conservative treatments such as rest, ice, physical therapy, and anti-inflammatory medications may be sufficient for healing. However, for more severe tears or those that cause persistent symptoms, surgical intervention may be necessary.
Surgical Options
Arthroscopic surgery is a common approach for repairing or removing the torn meniscus. During this minimally invasive procedure, a surgeon uses a tiny camera (arthroscope) and specialized instruments to address the meniscal tear. In cases where the meniscus cannot be repaired, a partial or total meniscectomy may be performed, where the damaged portion is removed.
Recovery and Rehabilitation
Recovery from a meniscal tear varies depending on the type of treatment received. Patients undergoing arthroscopic surgery can expect a shorter recovery period compared to those undergoing a meniscectomy. After surgery, physical therapy plays a crucial role in restoring knee strength, flexibility, and stability. Patients are advised to follow their doctor’s and physical therapist’s instructions diligently to achieve optimal outcomes.
Preventing Meniscal Tears
While not all meniscal tears can be prevented, certain measures can reduce the risk of injury. Maintaining strong thigh muscles through regular exercise can help stabilize the knee joint. Using proper techniques and protective gear during sports activities can also lower the risk of trauma-related tears.
A meniscal tear can significantly impact an individual’s daily life and athletic performance. Understanding the causes, symptoms, and treatment options for meniscal tears is essential for prompt diagnosis and effective management. Whether through conservative treatments or surgical intervention, successful recovery from a meniscal tear is possible with proper care and guidance from healthcare professionals. Remember to prioritize knee health, seek medical attention for any knee-related concerns, and adopt preventive measures to safeguard against potential injuries. With the right approach, you can effectively manage a meniscal tear and return to a healthy, active lifestyle.
3. Osteoarthritis

Understanding, Managing, and Living with Joint Degeneration
Osteoarthritis (OA) is the most prevalent form of arthritis and a leading cause of joint pain and disability. It occurs when the protective cartilage that cushions the ends of bones gradually wears down, leading to joint degeneration. OA can affect any joint in the body but is most common in weight-bearing joints such as the knees, hips, and spine. In this comprehensive article, we will delve into the causes, symptoms, diagnosis, and various treatment options available to manage osteoarthritis effectively.
Understanding Osteoarthritis
Osteoarthritis is a degenerative joint disease that primarily affects older adults, although it can also occur in younger individuals due to injury or other factors. As the cartilage wears away, bones may rub against each other, causing pain, swelling, and reduced joint flexibility. Over time, this can lead to significant mobility issues and a reduced quality of life.
Causes of Osteoarthritis
The exact cause of osteoarthritis is not fully understood, but several factors contribute to its development. Age, genetics, joint injuries, and excessive joint stress are common risk factors. Obesity and certain metabolic disorders can also increase the likelihood of developing OA. Understanding these risk factors can help individuals adopt preventive measures and manage the condition effectively.
Symptoms of Osteoarthritis
The symptoms of OA can vary depending on the affected joint and the stage of the disease. Common symptoms include joint pain, stiffness, tenderness, and reduced range of motion. As the condition progresses, individuals may experience joint swelling and the formation of bone spurs around the affected joint.
Diagnosing Osteoarthritis
Diagnosing osteoarthritis typically involves a combination of medical history, physical examination, and imaging tests such as X-rays and MRIs. These tests help doctors assess the condition of the affected joint and rule out other potential causes of joint pain and inflammation.
Treatment Options
While there is no cure for osteoarthritis, various treatment options can effectively manage the symptoms and improve joint function. Treatment plans are typically tailored to each individual’s needs and may include a combination of lifestyle changes, physical therapy, medications, and in some cases, surgical intervention.
Lifestyle Modifications
Lifestyle modifications play a vital role in managing OA. Maintaining a healthy weight through diet and exercise can help reduce stress on weight-bearing joints. Low-impact exercises such as swimming, cycling, and tai chi can improve joint flexibility and strengthen surrounding muscles.
Physical Therapy
Physical therapy is an essential component of osteoarthritis management. A physical therapist can design a personalized exercise program to improve joint range of motion, strength, and stability. They can also provide guidance on using assistive devices, such as braces or canes, to support affected joints.
Medications
Over-the-counter pain relievers and anti-inflammatory medications can help manage pain and inflammation associated with osteoarthritis. In some cases, doctors may prescribe stronger medications or corticosteroid injections to provide relief from severe joint pain.
Surgical Options
For individuals with advanced OA and significant joint damage, surgical intervention may be necessary. Joint replacement surgery, such as knee or hip replacement, can provide lasting pain relief and improved joint function.
Living with Osteoarthritis
Living with osteoarthritis requires proactive self-care and regular medical check-ups. Engaging in regular physical activity, managing stress, and adopting joint-friendly habits can enhance overall well-being. It’s essential to stay informed about the latest treatment options and lifestyle recommendations to make informed decisions about managing OA effectively.
Osteoarthritis is a prevalent joint condition that can impact daily life and limit physical activity. Understanding its causes, symptoms, and available treatment options is crucial for effectively managing the condition and maintaining joint function. By adopting healthy lifestyle practices, seeking medical guidance, and following a comprehensive treatment plan, individuals with OA can continue to lead fulfilling lives with reduced pain and improved joint mobility. Remember, early diagnosis and proactive management are key to living well with osteoarthritis and promoting overall joint health.
4. Ligament Sprains could be a cause for why Knee Hurts When Bent

Causes, Symptoms, Treatment, and Recovery
Ligament sprains are common injuries that occur when the strong bands of tissue connecting bones are stretched or torn. These sprains can range from mild to severe, causing pain and limiting joint mobility. Understanding the causes, symptoms, and treatment options for ligament sprains is essential for prompt and effective recovery. In this article, we’ll delve into the world of ligament sprains and explore ways to manage pain, promote healing, and prevent future injuries.
Understanding Ligament Sprains
Ligaments play a crucial role in stabilizing joints and preventing excessive movement. However, sudden twists, impacts, or overstretching can lead to ligament sprains. The severity of a sprain depends on the degree of ligament tearing, with mild sprains involving minimal tearing, while severe sprains may completely rupture the ligament.
Causes of Ligament Sprains
Ligament sprains can result from various factors, including sports injuries, falls, and accidents. Engaging in high-impact activities without proper warm-up and conditioning can increase the risk of sprains. Athletes and individuals involved in physically demanding activities should take precautionary measures to protect their ligaments and joints.
Symptoms of Ligament Sprains
The symptoms of a ligament sprain may include pain, swelling, bruising, and joint instability. Depending on the affected joint, individuals may have difficulty bearing weight or moving the joint through its full range of motion. Prompt recognition of these symptoms is crucial for timely treatment and preventing further damage.
Diagnosing Ligament Sprains
Diagnosing a ligament sprain involves a thorough physical examination and may require imaging tests such as X-rays or MRI scans. A healthcare professional will assess the extent of ligament damage to determine the appropriate course of treatment.
Treatment Options
The treatment for ligament sprains depends on the severity of the injury and the affected joint. In most cases, conservative treatments are sufficient for mild to moderate sprains, while severe sprains may require surgical intervention.
Rest and Immobilization
Resting the injured joint and immobilizing it with a brace or splint is essential for the initial phase of recovery. Avoiding activities that put stress on the injured ligament allows it to heal properly.
Ice and Compression
Applying ice to the affected area can help reduce swelling and inflammation. Compression bandages can also provide support and limit swelling.
Elevation
Elevating the injured limb above heart level can reduce swelling by promoting better blood flow and fluid drainage.
Physical Therapy
Physical therapy plays a crucial role in ligament sprain recovery. A skilled therapist can design a personalized exercise program to improve joint strength, stability, and range of motion.
Pain Management
Over-the-counter pain relievers and anti-inflammatory medications can help manage pain and reduce inflammation during the healing process.
Surgical Intervention
For severe ligament sprains that do not respond to conservative treatments, surgical repair may be necessary. Surgical techniques can vary depending on the location and extent of ligament damage.
Recovery and Prevention
Recovering from a ligament sprain requires patience and adherence to the treatment plan. Gradual return to physical activity, under the guidance of a healthcare professional, is essential to prevent re-injury.
Preventing Future Ligament Sprains
Preventing ligament sprains involves proper warm-up before physical activity, using appropriate protective gear, and maintaining good physical fitness and flexibility.
Ligament sprains are common injuries that can be painful and limit joint mobility. Understanding the causes, symptoms, and treatment options for ligament sprains is essential for effective recovery and prevention of future injuries. Whether through conservative treatments or surgical intervention, early and appropriate management can lead to a successful recovery and a return to an active and healthy lifestyle. By taking preventive measures and seeking prompt medical attention when needed, individuals can protect their ligaments and enjoy a life free from the limitations of ligament sprains.
Knee Hurts When Bent: Tips for Managing
If you’re experiencing knee pain when bending, there are several tips you can follow to find relief:
1. Rest and Elevation: Give your knee sufficient rest and elevate it to reduce swelling and promote healing.
2. Ice and Heat Therapy: Apply ice packs to reduce inflammation and pain in the acute stage, and use heat therapy to relax the muscles and improve blood circulation in the later stages.
3. Gentle Stretching and Strengthening Exercises: Engage in exercises recommended by a healthcare professional or physical therapist to improve knee flexibility, strength, and stability.
4. Pain Medications and Anti-inflammatory Drugs: Over-the-counter pain relievers and anti-inflammatory medications can help alleviate pain and reduce inflammation.
When to Seek Medical Attention
While mild knee pain can often be managed with self-care measures, there are instances when medical attention is necessary. Consider consulting a healthcare professional if:
- The pain is severe and persistent
- There is significant swelling or redness
- The knee feels unstable or gives way frequently
- You have difficulty bearing weight on the affected knee
Prompt medical evaluation is crucial to determine the underlying cause and establish an appropriate treatment plan.
Preventive Measures for when Knee Hurts When Bent
Prevention is key to avoiding knee pain when bending. Here are some preventive measures to consider:
1. Maintaining a Healthy Weight: Excess weight places additional stress on the knee joint. Maintaining a healthy weight can reduce the risk of knee pain and related complications.
2. Using Proper Form During Physical Activities: Ensure proper technique and form during exercises and activities to minimize strain on the knees.
3. Wearing Appropriate Footwear: Choose footwear with good cushioning and support to absorb shock and reduce stress on the knees.
4. Regular Exercise and Conditioning: Engage in regular low-impact exercises, such as swimming or cycling, to strengthen the muscles around the knee and improve joint stability.
Lifestyle Modifications
Certain lifestyle modifications can also contribute to reducing knee pain when bending. Consider the following:
1. Dietary Changes for Joint Health: Incorporate foods rich in omega-3 fatty acids, antioxidants, and nutrients that support joint health, such as fish, nuts, berries, and leafy greens.
2. Incorporating Low-Impact Exercises: Choose low-impact activities that put less stress on the knees, such as yoga or Pilates, to maintain flexibility and strengthen supporting muscles.
3. Avoiding Excessive Kneeling or Squatting: Minimize activities that involve prolonged kneeling or deep squatting to reduce strain on the knee joint.
Coping Strategies for Daily Activities
Adopting specific coping strategies can help manage knee pain when engaging in daily activities. Consider the following:
1. Using Knee Braces or Supports: Utilize knee braces or supports to provide stability, reduce pain, and prevent further injury.
2. Modification of Activities to Reduce Knee Stress: Modify your movements and avoid activities that exacerbate knee pain, such as high-impact exercises or repetitive knee-bending motions.
3. Assistive Devices for Mobility Support: When necessary, use assistive devices like crutches or canes to alleviate pressure on the knee joint and aid mobility.
Seeking Professional Help
If knee pain persists or becomes increasingly challenging to manage, seeking professional help is crucial. A healthcare professional can provide an accurate diagnosis and recommend appropriate treatment options, which may include:
- Physical therapy and rehabilitation exercises
- Medications or injections for pain management
- Minimally invasive procedures or surgical interventions, if necessary
Conclusion
Experiencing knee pain when bending can significantly impact your daily life. By understanding the causes, implementing preventive measures, and following appropriate management strategies, you can find relief and improve the health of your knees. Remember to consult a healthcare professional for a thorough evaluation and personalized guidance.
FAQs
1. Can knee pain when bent be a sign of a serious condition?
While knee pain when bent can often be attributed to less severe issues, such as strain or minor injuries, it can sometimes indicate more serious underlying conditions. It’s essential to consult a healthcare professional for a proper diagnosis.
2. How long should I rest my knee if it hurts when bent?
The duration of rest depends on the severity and cause of your knee pain. It’s best to follow the guidance of a healthcare professional, who can assess your specific condition and provide appropriate recommendations.
3. Are there any exercises that can help alleviate knee pain when bending?
Gentle stretching and strengthening exercises, such as quadriceps and hamstring stretches, straight leg raises, and wall squats, can help alleviate knee pain. However, it’s important to consult a healthcare professional or physical therapist for personalized exercise recommendations.
4. Can wearing knee braces provide relief from knee pain when bending?
Knee braces can provide support, stability, and pain relief for certain conditions. However, it’s crucial to consult a healthcare professional to determine the most suitable type of knee brace for your specific needs.
5. Are there any natural remedies for knee pain when bent?
While natural remedies may provide temporary relief, it’s important to note that they may not address the underlying cause of the pain. However, some people find that practices such as applying heat or cold packs, using herbal ointments or creams, or practicing gentle yoga and meditation techniques can help manage knee pain. It’s always advisable to consult with a healthcare professional before trying any natural remedies.
Remember, if you’re experiencing persistent or severe knee pain when bent, it’s crucial to seek medical advice for an accurate diagnosis and appropriate treatment options.
*We may earn a commission from purchases made through our links, at no cost to you. This does not affect our product recommendations. Please see our disclosure to learn more.
![Urban Health Hive]](https://urbanhealthhive.com/wp-content/uploads/2023/05/cropped-cropped-Health_Logo.png)